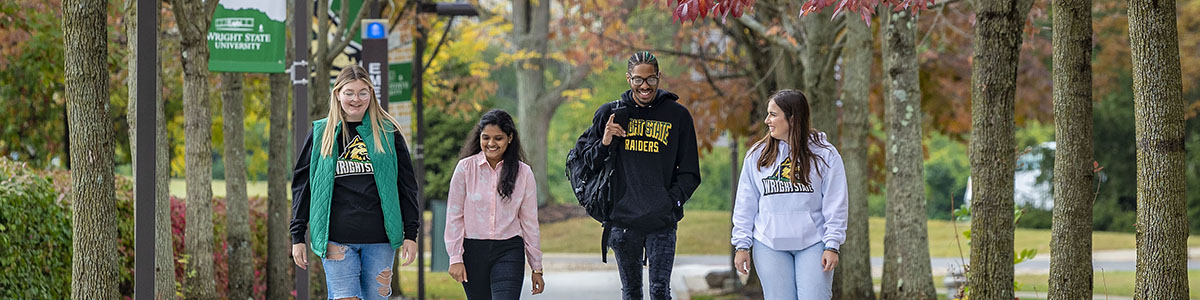We’re here to cultivate a flourishing Wright State University community.
triangle-exclamation Need Crisis Help Now?
If this is a life threatening emergency, call 911 or Public Safety at 937-775-2111.
Call Raider Cares at 937-775-4567
Call 988 for the Suicide and Crisis Lifeline
Chat 988 at 988lifeline.org
Text Suicide and Crisis Lifeline at 741741
Find emergency and essential resources
square-check Get a Check Up from your Neck Up?
Located in 053 Student Union, in the lower level just below the main entrance, Counseling and Wellness Services (CWS) offers a variety of services and resources to currently enrolled Wright State students including individual and group therapy, psychiatric services, and health promotion programming. Our staff, interns, and residents are here to support Wright State students in a safe, confidential, and inclusive space.
Our services are included in the Counseling and Wellness Services Fee on your university bill each semester. This is an optional $20 fee, which covers all mental health services at CWS for no additional cost for the semester. If you choose to waive the fee, CWS services are still available to you at the cost of $20 per session.
We strive to enhance Raider Wellness through our variety of services, including:
people-arrows
One-on-One Services
CWS provides individual counseling through our skilled team of psychologists, licensed staff counselors, social workers, interns and trainees.
people-group
Group Therapy
Did you know group counseling can be just as effective as individual therapy for some students? CWS offers several groups each semester that may be a good fit for you.
person-circle-exclamation
Walk-in/Crisis Services
We offer walk-in services during office hours to immediately connect with a provider for understanding and support.
person-circle-question
Faculty and Staff Consultation
Faculty and staff who have questions regarding student and administrative concerns can contact CWS at 937-775-3407. There are also additional resources available for faculty and staff who may want to assist a student.
person-chalkboard
Outreach and Education
CWS is dedicated to being an active presence in the Wright State community through outreach and health promotion efforts.
square-check
Get a Check Up from your Neck Up
Take a mental health screening today. The screening is completely anonymous. The screening has 36 questions. You will receive immediate results that will help you identify signs of distress. The Counseling and Wellness staff will be available to discuss your results. Contact us or make an appointment today.
people-arrows
Free Mental Health and Suicide Prevention Training
We know that suicide prevention can be a difficult topic, but when everyone on campus learns to recognize warning signs and help a student at risk, it can save lives. Take this 30-minute training to contribute to a safer and more supportive Wright State community.
camera Photos
View photos of our office and past events.
Mission and Vision
Counseling and Wellness Services (CWS) is the Wright State University student mental health and health promotion service.
Our Vision is to cultivate a flourishing Wright State University community.
Our Mission is to promote optimal student wellness and mental health and the pursuit of social justice through the provision of quality education, consultation, and clinical service and training as an active presence in the Wright State University community with an appreciation for multiculturalism and diversity.
Our Location
We are located in 053 Student Union.
Student Union Building Map (PDF)